The Challenge
St. Luke’s Health System provides high-quality care across big, mostly rural states, and is regularly challenged to connect medical professionals with remote care providers and their patients. Often, specialists based in Boise, Idaho need to drive five hours or more to smaller centers across the state to see patients directly, or mentor and advise remote St. Luke’s colleagues.
The Solution
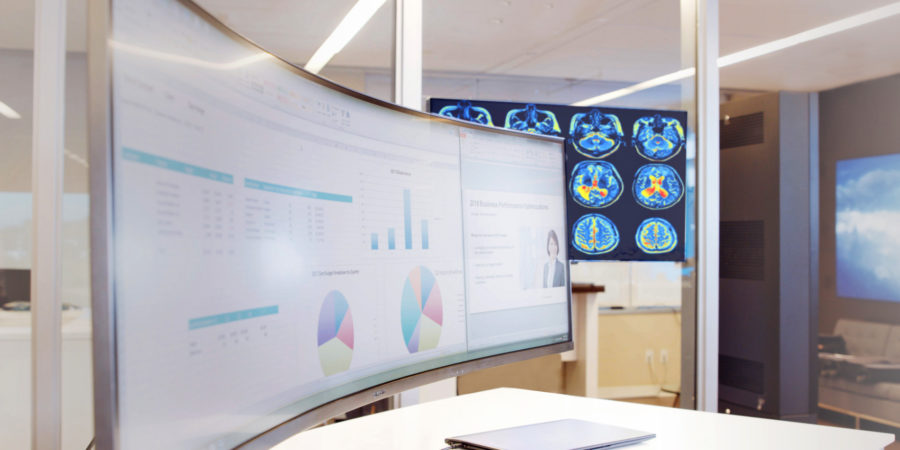
St. Luke’s has developed a 24/7 telehealth platform that connects remote patients and intensive care providers in smaller centers with nurses and specialist physicians, operating from a specially designed Boise facility. Using videoconferencing and built around extra-wide, immersive 49-in. monitors, service providers now offer virtual care and advice for patients and caregivers that bridge distances and greatly reduce wait times.
The 49-inch curved monitor provides enough surface area for all necessary applications to be seen at once.

About St. Luke's Health System
St. Luke’s Health System is Idaho’s largest employer, with a medical staff of more than 1,800 physicians and advanced practice providers. Based in Boise, St. Luke’s has eight hospitals around central and southern Idaho. It is the only locally owned and operated, physician-led, not-for-profit health system in the state. Truven Health Analytics has named St. Luke’s among the top 15 health systems in the U.S. five times.
The Challenge
Closing Distances for Caregivers and Patients
The lack of local access to medical specialists is a common problem in small cities, towns and villages across the U.S. and other countries. Seeing a specialist can mean long drives or even plane flights to larger population centers, or scheduling appointments locally when a specialist makes a periodic visit to a smaller center.
Access to good advice and guidance is also a challenge for patient-facing caregivers in scenarios like intensive care units, where doctors and nurses may have little or no experience with injuries or illnesses rarely seen at their rural facilities.
Phone calls and emails offer limited solutions, but healthcare providers have started applying more sophisticated technology to bridge distances and connect both patients and their caregivers with expert advice, insight and direction.
While St. Luke’s Health System has a main facility in Boise, its other locations serve smaller centers that are, in some cases, hours away by car. Specialists like oncologists and cardiologists have full-time demands in Boise, and getting direct patient appointments with them involves either traveling to the capital, or waiting for specialists to schedule one of their occasional visits to a smaller center.
To make care more accessible, St. Luke’s developed a dedicated virtual care center in Boise that connects nurses with rural care providers and their patients, using web-based videoconferencing, custom software, cameras, microphones and display monitors. The 24/7 facility enables nurses to see and speak with patients and simultaneously review tests on screens at their workstations. Specialists also use the virtual care stations to “meet” with patients and colleagues to review cases without leaving Boise. They can schedule time, have their meetings and be back on ward floors in a matter of minutes.
A version of the virtual care facility is dedicated to intensive care. Workstations with multiple displays allow deeply experienced care providers and specialists to monitor and contribute to acute care situations in remote locations. With access to video, audio, patient records and vital stats, remote caregivers can coach locals on how to deal with medical situations — such as illnesses or injuries — they only rarely encounter in the smaller center.
These virtual care stations in Boise were originally set up with groups of three monitors or, for intensive care stations, as many as six, stacked three on three. The setup was a high maintenance tangle of power and signal cables that resulted in a large viewing canvas bisected by the doubled-up frames of each screen.
It worked, but left a lot of room for improvement.
The Solution
Immersive Monitors Lower Costs and Improve Experiences
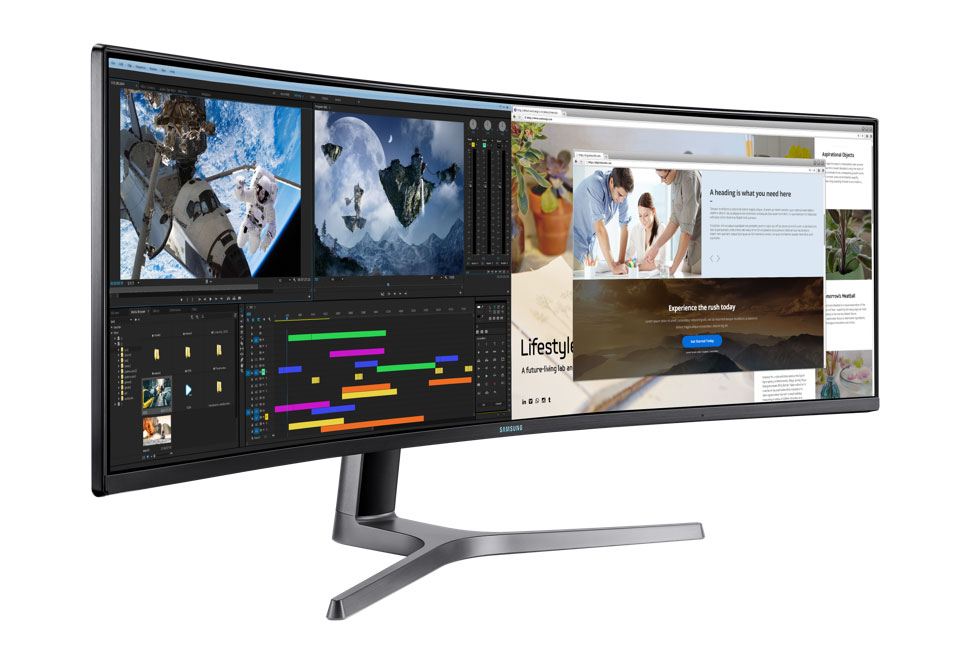
Starting in 2018, St. Luke’s began rolling over the workstations to a new setup that uses Samsung 49-in. curved monitors. The extra-wide displays simplify the number and management of cables, remove much of the metal mounting array needed at desks and provide one big, continuous screen with no breaks.
Richard Eidemiller, the IT solutions architect at St. Luke’s who has guided the transition to extra-wide curved screens, says the switch had obvious benefits:
- Lower costs: The aggregate cost of one versus three screens was lower, particularly when the need for additional mounting hardware was removed. With fewer displays, energy consumption and its costs were also reduced.
- Less weight: The combination of one light LCD display and the reduction of metal mounting brackets reduced the weight impact on desks.
- Lower maintenance: Simple and minimal connections means fewer cables to manage and less desktop support required from IT teams.

- Standardization: Instead of specialized computers with dedicated graphics cards needed to drive the old display setup, the 49-in. screens are now driven by standard PCs used widely across the St. Luke’s system. Standardized PCs are more easily and readily supported by St. Luke’s IT teams.
- Better experience: The immersive design of curved displays reduces eye strain for power-users, and allows caregivers to easily load a remote camera view, patient records and other hospital care applications on a single screen, with no need to minimize any windows.
“We wanted to give the users a good, immersive setup, because the nurses are looking at screens for 12 hours a day,” says Eidemiller. “It’s something that they can comfortably look at, as well as present enough information across the screens that they need to see.”
When planning out the hardware setup, Eidemiller considered more conventional widescreen monitors, but was drawn to Samsung’s 49-in. screens because of the sheer breadth of viewing canvas and its curved design that means the content at the left and right edges is as close to viewer eyes as the center.
“I go to tech convention healthcare trade shows,” says Eidemiller, “and what I didn’t like about the flat-screen monitors I’d see is that, when you are close to normal, flat widescreen monitors, your viewing angle is thrown off. It looks a little funny.”
Ten virtual care stations at St. Luke’s use a pair of 49-in. curved widescreens, one stacked atop the other. There are more than 40 other stations using a single curved widescreen.
The new widescreen setup also provides a degree of future-proofing. “I wanted to buy technology today that we can use for many years, and these monitors seem to fit that bill,” says Eidemiller. “We can grow into them, versus having to find a different solution and replace perfectly good equipment with new equipment down the road.”

The Technology
CJ890 Series 49" Curved
Large 49-inch super ultra-wide 32:9 curved monitor with USB-C and KVM switch and screen splitting capabilities.
The Results
Virtual Care Just the Start for Widescreen Adoption
The virtual care center is running full-time with nurses on 12-hour shifts, and physicians are gradually embracing the concept of remote care versus face-to-face, the latter only being possible at the end of a long travel day.
“We’re trying to lure them,” says Eidemiller, “suggesting they start seeing remote patients this way, reducing their drive times and increasing the amount of patients they can see during that period of time.
“Some people have already embraced the new system,” he adds. “They pick a day of the week or a couple of days out of the month, and use this technology. And that’s going to be ramping up. We’re going to start requiring that more and more of the physicians use the technology, versus just driving everywhere.”
St. Luke’s investment in Samsung widescreens is so far limited to delivering telehealth, but Eidemiller expects wider adoption to follow both in patient care stations around facilities and in back office and administration areas where users would benefit from wide, ergonomically friendly displays that allow for multitasking or full views of important information such as broad spreadsheets, construction drawings and project management documents.
Eidemiller says as awareness around St. Luke’s has grown, so has interest in using the big screens.
“I haven’t met a person who wouldn’t be excited,” he says. “We’ve had state legislators come through, we’ve had other hospital systems, other organizations. As people come through and see them, they find other applications outside of how we are specifically using them.
“I don’t have enough spares to loan out to everybody who wants one of these, but as they become available, I let them know. People are eager to take them,” he muses.
“It’s getting them back that’s the hard part.”